People.unipmn.it
A Hybrid Approach to Clinical Guideline and to
Basic Medical Knowledge Conformance
A. Bottrighi1, F. Chesani2, P. Mello2, G. Molino3, M. Montali2, S. Montani1,
S. Storari4, P. Terenziani1, and M. Torchio3
1 DI, Univ. del Piemonte Orientale, via Bellini 25/g, 15100 - Alessandria, Italy
2 DEIS - Univ. di Bologna, viale Risorgimento 2, 40136 - Bologna, Italy
3 Az. Ospedaliera S. Giovanni Battista, via Bramante 88, Torino, Italy
4 DI - Univ. di Ferrara, via Saragat 1, 44136 - Ferrara, Italy
Abstract. Several computer-based approaches to Clinical Guidelineshave been developed in the last two decades. However, only recently thecommunity has started to cope with the fact that Clinical Guidelinesare just a part of the medical knowledge that physicians have to takeinto account when treating patients. The
procedural knowledge in theguidelines have to be complemented by additional
declarative medicalknowledge. In this paper, we analyse such an interaction, by studyingthe conformance problem, defined as evaluating the adherence of a setof performed clinical actions w.r.t. the behaviour recommended by theguideline and by the medical knowledge.
Clinical Guidelines are "systematically developed statements to assist practi-tioner and patient decisions about appropriate health care for specific clinicalcircumstances" [4]. In the last decade, the research about computerized guide-lines has reached a relevant role within the Artificial Intelligence in Medicinecommunity, and many different approaches and projects have been developedto create domain-independent computer-assisted tools for managing, acquiring,representing and executing clinical guidelines [8]. Only recently, however, someapproaches have started to consider that Clinical Guidelines (henceforth CG)cannot be interpreted (and executed) "in isolation". CGs are just a part of themedical knowledge that physicians have to take into account when treating pa-tients. The
procedural knowledge in the guidelines have to be complemented byadditional
declarative medical knowledge. In this paper we explore such an inter-action from the viewpoint of the conformance problem, intended as the adherenceof an observed execution to both types of knowledge.
Guidelines, Basic Medical Knowledge and Conformance
Several conditions are usually implicitly assumed by experts building a CG:
(
i)
ideal patients, i.e., patients that have "just the single" disease considered in
the CG (thus excluding the concurrent application of more than one CG),and are "statistically relevant" (they model the typical patient affected bythe given disease), not presenting rare peculiarities/side-effects;
(
ii)
ideal physicians executing the CG, i.e., physicians having the basic medical
knowledge, allowing them to properly apply the CGs to specific patients;
(
iii)
ideal context of execution, so that all necessary resources are available.
Assumption (
i) is needed, since the variety of possible patients is potentially infi-nite, and the CG cannot explicitly cope with all possible nuances and exceptions.
Assumption (
ii) is also necessary, since the CG focuses on the proper treatmentof a specific disease, and can not code all the "basic medical knowledge". Nev-ertheless, such a knowledge is needed when a CG will be executed, to properlyadapt the "general" prescriptions in the CG to the specific case constituted by aparticular patient. Finally, experts cannot know all possible execution contexts,so that they usually assume availability of resources (assumption (
iii)).
As a consequence of these assumptions, a CG cannot be interpreted as a
protocol which has to be applied tout cour, and the actions prescribed by CGscannot be interpreted as "must do" actions. The intended semantics of CGs can-not be analysed in isolation from the
basic medical knowledge. Roughly speaking,given a patient
X to which a CG
G has to be applied in a context
C,
G has tobe interpreted as a set of
default prescriptions: whenever
X and
C fit with
G'sprescriptions, they must be executed. However,
X (or
C) may have peculiar fea-tures which are not explicitly covered by
G. In such a case, the
basic medicalknowledge must be considered to identify the correct actions.
The interplays between CG's knowledge and the Basic Medical Knowledge
(BMK from now on) can be very complex, as shown by the following examples.
Example 1. Patients suffering from bacterial pneumonia caused by agents sen-sible to penicillin and to macrolid, allergic to penicillin, must be treated withmacrolid.
BMK: Don't administer drug X to a patient if she is allergic to X.
In Ex. 1, two alternative treatments (penicillin or macrolid) are possible given theCG, but one of them is excluded, given the underlying basic medical knowledge,because of allergy to penicillin. Here the BMK "complete" the CG and helpto discriminate among different alternatives. In other cases, the basic medicalknowledge may apparently contradict the recommendations in the CG.
Example 2. Patient with acute myocardial infarction presenting with acute pul-monary edema; before performing coronary angiography it is mandatory to treatthe acute heart failure.
BMK: The execution of any CG may be suspended, if a problem threatening thepatient's life suddenly arise. Such a problem has to be treated first.
In Ex. 2 the execution of a CG is suspended, due to the arise of a problemthreatening the patient's life. Notice that the "contradiction" (logical inconsis-tency) between CG's recommendations and BMK is only apparent. It arises justin cases one interpret CG's recommendations as
must do, while, as a matter offacts, they may be emended by BMK.
Also, there seems to be no general rule in case of "apparent contradiction":
it could be that BMK recommendations "win" over CG ones, or vice versa. InEx. 3 a treatment is performed even if it may be dangerous for the patient. Insome sense, not only some CG's prescriptions are "defeasible", since they maybe overridden by BMK, but the same also holds for part of BMK.
Example 3. In a patient affected by unstable angina and advanced predialytic re-nal failure, coronary angiography remains mandatory, even if the contrast mediaadministration may cause a further final deterioration of the renal functions,leading the patient to dialysis.
When considering conformance of an execution w.r.t. a CG, additional ac-
tions not foreseen by the CG could be considered as an issue. This could happenas a consequence of some particular routine (even a CG applied at the sametime), like in Ex. 4.
Example 4. Calcemia and glycemia are routinely performed in all patients admit-ted to the internal medicine ward of Italian hospitals, regardless of the disease.
To summarize, CG semantics is very complex, and cannot be simply inter-
preted as a strict, normative procedures. The context of execution and the BMKcomplement the prescriptions in the CGs, bridging (at least in part) the gap be-tween the "ideal" and the "real" application cases. In this hybrid situation theproperty of conformance, intended as the adherence of an execution to CGs andBMK recommendation, becomes more and more important, and yet difficultto be captured. Defining conformance as the simple conjunction of the confor-mances to each different piece of knowledge might not be the best choice. Boththe CG knowledge and the BMK can be defeated, hence there is no general ruleon the prevalence of one or the other. The conformance evaluation is a task that
necessarily requires the intervention of a physician. However, such a task can bevery difficult and time consuming.
Evaluating Conformance
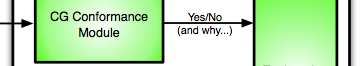
We propose to combine, in an hybrid system, tools used for independently evalu-ating conformance to CGs and BMK. The aim is twofold: on one side, we combineboth types of knowledge; on the other side, we facilitate the physician task byidentifying discrepancies between actual executions and CG/BMK recommen-dations, and by suggesting possible explanations. The architecture is shown inFigure 1.
Procedural and workflow-like systems seems to be the most common choice
for representing CGs [6], while declarative approaches might be preferable to





Clinical Guideline
Patient Execution
Basic Medical Knowledge
Fig. 1. Architecture of our hybrid approach for the conformance evaluation
represent BMK, due to its similarity to knowledge bases. Our system takes asinput three different pieces of information: a CG described using the GLARElanguage [9], a BMK described by means of the SCIFF language [1], and a set ofdata about the patient (the "Patient DB"). The Patient DB includes the patientdata (a description of the patient and her medical situation); and the actualexecution (a list of the medical actions executed on that patient).
The conformance is evaluated by means of two different modules, and their
output is combined to provide possible explanations. The first module is theCG Conformance Module. It compares the observed execution with the "ideal"execution, to spot possible differences:(i) executed actions not envisaged by theCG, and (ii) actions foreseen by the CG but not observed in the execution. Theideal execution is obtained through the GLARE system, by applying specificpatient data to the generic CG description.
The second module, the BMK Conformance Module, tests the conformance
of the actual execution w.r.t. the BMK, expressed using the SCIFF formalism.
The SCIFF Proof Procedure generates expectations about the events, and au-tomatically checks if such expectations are fulfilled or not. Besides a yes/noanswer, the SCIFF Proof Procedure provides also explanations, in terms of theexpectations about the happened/not happened events.
Finally, the Explanation Module combines the outputs of the two previ-
ous modules: a list of discrepancies (observed/not observed medical actions)is given to the physician, together with expectations that might justify the pres-ence/absence of the observed discrepancies.
Several proposals for representing CGs have been made: in [6, 8] the interestedreader can find surveys and comparisons of the many formalisms. Recently, therehas been a growing interest in declarative paradigms for modeling process mod-els. In [5] the declarative language CIGDEC for clinical guidelines is presented.
CIGDEC lets the user to define constraints that must hold among activities ex-ecution, but integration with procedural specifications are not considered. In [3]the authors integrate the domain knowledge within an adaptive Process Man-agement System (PMS), by means of semantic constraints. A generic criterionfor semantic correctness of processes is given. However, unlike SCIFF seman-tic constraints can not take into account contexts, time, locations and data ingeneral.
In [7] the problem of augmenting CG rules with collateral medical information
was first pointed out. More recently, in Protocure and Protocure II EU projectsthere has been an extensive attempt to couple CGs and BMK. CGS are modeledusing Asbru, while the BMK is given as a set of formulas in future-time LTL.
The theorem prover KIV is used to perform quality checks [2], focussing onproperties of CG "per se", and ignoring the conformance dimension.
Acknowledgements. This work has been partially supported by the FIRB projectTOCAI.it (RBNE05BFRK) and by the Italian MIUR PRIN 2007 project No.
20077WWCR8.
1. M. Alberti, F. Chesani, M. Gavanelli, E. Lamma, P. Mello, and P. Torroni. Verifiable
agent interaction in abductive logic programming: the SCIFF framework. ACMTransactions on Computational Logics, 9(4), 2008.
2. A. Hommersom, P. Groot, P.J.F. Lucas, M. Balser, and J. Schmitt. Verification of
medical guidelines using background knowledge in task networks. Knowledge andData Engineering, IEEE Transactions on, 19(6):832–846, June 2007.
3. L. T. Ly, S. Rinderle, and P. Dadam. Integration and verification of semantic
constraints in adaptive process management systems. Data Knowl. Eng., 64(1):3–23, 2008.
4. Field MJ and Lohr KN, editors. Clinical Practice Guidelines: Directions for a New
Program. Institute of Medicine, Washington, DC, National Academy Press, 1990.
5. N. Mulyar, M. Pesic, W. M. P. van der Aalst, and M. Peleg. Declarative and
procedural approaches for modelling clinical guidelines: Addressing flexibility issues.
In BPM Workshops, volume 4928 of LNCS, pages 335–346. Springer, 2007.
6. M. Peleg, S. Tu, J. Bury, P. Ciccarese, N. Jones, J. Fox, R. A. Greenes, R. Hall, P.D.
Johnson, N. Jones, A. Kumar, S. Miksch, S. Quaglini, A. Seyfang, E. H. Shortliffe,and M. Stefanelli. Comparing computer-interpretable guideline models: A case-study approach. JAMIA, 10(1), 2003.
7. R. N. Shiffman. Representation of clinical practice guidelines in conventional and
augmented decision tables. J Am Med Inform Assoc, 4(5):382–393, Sep-Oct 1997.
8. A. Ten Teije, S. Miksch, and P. Lucas, editors. Computer-based Medical Guide-
lines and Protocols: A Primer and Current Trends, volume 139 of Studies in HealthTechnology and Informatics. IOS Press, Amsterdam, July 2008.
9. P. Terenziani, S. Montani, A. Bottrighi, G. Molino, and M. Torchio. Applying
Artificial Intelligence to Clinical Guidelines: the GLARE Approach. Volume 139 ofTeije et al. [8], July 2008.
Source: http://people.unipmn.it/stefania/papers-pdf/C79.pdf
LEY Nº 18.045 (1) LEY DE MERCADO DE VALORES Objetivos de la ley, fiscalización y definiciones Artículo 1°.- A las disposiciones de la presente ley queda sometida la oferta pública de valores y sus respectivos mercados e intermediarios, los que comprenden las bolsas de valores, los corredores de bolsa y los agentes de valores; las sociedades anónimas abiertas; los emisores e instrumentos de oferta pública y los mercados secundarios de dichos valores dentro y fuera de las bolsas, aplicándose este cuerpo legal a todas aquellas transacciones de valores que tengan su origen en ofertas públicas de los mismos o que se efectúen con intermediación por parte de corredores o agentes de valores.
2016–2017 TBOR Basic International Student Injury and Sickness Plan Endorsed by Middle Tennessee State University Who is eligible to enroll? How do I Enroll? International students or other persons with a current To enroll visit www.pghintlstudent.com, and follow passport who: 1) are engaged in educational activities; 2) are temporarily located outside his/her home country as a















